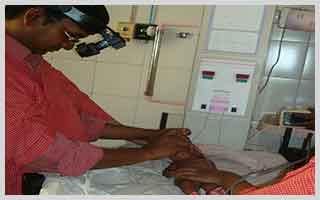
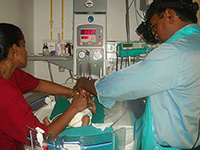
ROP Screening guidelines
With improvement in neonatal care and survival of very low birth weight babies in India, there is an alarming increase in the incidence of retinopathy of prematurity (ROP). While the problem is on the decline in developed countries due to robust screening programs in place, most developing countries including India are presently experiencing the “third epidemic” of ROP. One of the most important steps in tackling this giant is to have an appropriate and effective screening strategy. Herein, we elucidate the ROP screening guidelines suitable for developing countries like India.
The primary objective of screening is to detect ROP at a time that is appropriate for treatment.
What is screening window in ROP?
Natural history data from studies have shown that Progression of ROP follows a distinct sequence according to the post-menstrual age (PMA) of the baby.
Retinal findings indicative of poor outcome are seen in only 1% of infants before 31 weeks PMA and in only 1% of infants after 46.3 weeks PMA. The median age for detection of stage 1 ROP is 34 weeks. Pre-threshold ROP appears at 36 weeks of post-menstrual age and threshold disease at 37 weeks. Vascularization is complete by 40 weeks of gestation.
Thus the crucial period for detection of ROP is from 32 weeks to 40 weeks of post-menstrual period. The critical phase is from 34-35 weeks to 37-38 weeks age during which the progression of the disease takes place and treatment may have to be instituted.
Which babies need to be screened?
- Babies with birth weight <1500 g
- Babies born at ≤32 weeks of gestation
- Selected preterm infants with a birth weight between 1500 and 2000 g or gestational age of more than 32 weeks with an unstable clinical course, including those requiring cardiorespiratory support and who are believed by their attending pediatrician or neonatologist to be at high risk, should have retinal screening examinations
Who should perform the screenings?
Retinal examinations in preterm infants should be performed by an ophthalmologist who has sufficient knowledge and experience to enable accurate identification of the location and sequential retinal changes of ROP.
When should the screening be started?
The initiation of acute-phase ROP screening should be based on the infant’s age. The onset of serious ROP correlates better with postmenstrual age (gestational age at birth plus chronologic age) than with postnatal age.
First screening examination should be carried out at 31 weeks of gestation or 4 weeks of age, whichever is earlier
|
Gestational Age at Birth, wk |
Age at Initial Examination, wk |
|
|
Postmenstrual |
Chronologic |
|
|
22 |
31 |
9 |
|
23 |
31 |
8 |
|
24 |
31 |
7 |
|
25 |
31 |
6 |
|
26 |
31 |
5 |
|
27 |
31 |
4 |
|
28 |
32 |
4 |
|
29 |
33 |
4 |
|
30 |
34 |
4 |
|
31 |
35 |
4 |
|
32 |
36 |
4 |
How often should the babies be followed up?
Follow-up examinations should be recommended by the examining ophthalmologist on the basis of retinal findings classified according to the international classification. The following schedule is suggested:
1-week or less follow-up
- stage 1 or 2 ROP: zone I
- stage 3 ROP: zone II
1- to 2-week follow-up
- immature vascularization: zone I—no ROP
- stage 2 ROP: zone II
- regressing ROP: zone I
2-week follow-up
- stage 1 ROP: zone II
- regressing ROP: zone II
2- to 3-week follow-up
- immature vascularization: zone II—no ROP
- stage 1 or 2 ROP: zone III
- regressing ROP: zone III
Where should the babies be screened?
Neonates are best examined in the NICU itself under supervision of attending pediatrician. It is best to avoid shifting small babies to ophthalmic outpatient department or ward for examination.
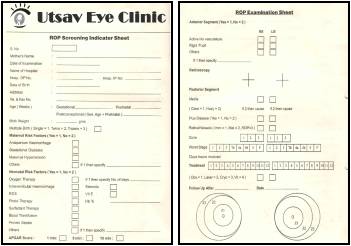
How to record findings during screening?
Ophthalmological notes should be made after each ROP examination, detailing zone, stage and extent in terms of clock hours of any ROP and the presence of any pre-plus or plus disease. These notes should include a recommendation for the timing of the next examination (if any) and be kept with the baby’s medical record.
Click here to download the ROP Screening Sheet
Which babies require treatment?
Treatment may be initiated for the following retinal findings:
- zone I ROP: any stage with plus disease
- zone I ROP: stage 3—no plus disease
- zone II: stage 2 or 3 with plus disease
- Plus disease is defined as a degree of dilation and tortuosity of the posterior retinal blood vessels as defined by a standard photograph. Special care must be used in determining the zone of disease. Treatment should generally be accomplished, when possible, within 72 hours of determination of treatable disease to minimize the risk of retinal detachment.
When can ROP screenings be concluded?
The conclusion of acute retinal screening examinations should be based on age and retinal ophthalmoscopic findings. Findings that suggest that examinations can be curtailed include the following:
- zone III retinal vascularization attained without previous zone I or II ROP (if there is examiner doubt about the zone or if the postmenstrual age is less than 35 weeks, confirmatory examinations may be warranted);
- full retinal vascularization;
- postmenstrual age of 45 weeks and no prethreshold disease (defined as stage 3 ROP in zone II, any ROP in zone I) or worse ROP is present; or
- regression of ROP (care must be taken to be sure that there is no abnormal vascular tissue present that is capable of reactivation and progression).